Bringing a child into the world is such a blessing. For me, it was a blessing beyond words since I had been told I would never get pregnant. We were beyond excited when we learned that we would be parents but then she sent me to the hospital in premature labor at just 23 weeks gestation. Our journey for the next 5 months would be scary, joyful, frustrating, and miraculous and would ultimately give me a different perspective as a parent to a micro-premie that I believe makes me a better SLP.
1. ALWAYS FIND and SHARE THE POSITIVE and NOT JUST THE FACTS.
During our month stuck in the hospital bed, the hospital had to visit me multiple times to share with me the facts of what could go wrong if my baby was delivered at that time. Now, I am all for being brutally honest and I even understand that the hospital had to give me the facts and make sure I understood. I even get that they had to have my sign the paper stating they went over the consequences of my medical situation. However, the constant highlight of all that could be wrong (even when I told them I had been in special education for so many years and knew the statistics) sent me in a spiral of negative which resulted in my emotionally pulling away from the child in womb. I was so scared of losing her that I found myself falling into a depressive state and detaching emotionally so that any loss that might occur might hurt less (a ridiculous thought from a depressive state). So we need to remember to shine the light of positivity on situations. Highlight whatever silver lining we can find and celebrate all the accomplishments including the little ones!
I get it. Sometimes, parents make our job more difficult. Sometimes, our feathers are a little ruffled because we think they do not respect our professional opinion. Whatever the reason, take a deep breath and remember we are a team with that advocating parent. They are fighting for the best services for their child. Sometimes those services are not warranted or appropriate but they do not always know that. They simply want to make sure we are doing everything we can for their child. I learned this as a parent that needed to advocate for my own child when the hospital wanted to move her to another hospital but I refused to do so until they had donor milk at the new hospital for her. I know I was a thorn in both hospital’s sides because I refused for 2 weeks to move my child until they had the donor milk. In the end, my refusal resulted in the second hospital getting the donor milk and my child was the first to receive this service at that location and it provided her with important nutrients that I could not provide nor could formula provide for my micro-preemie.
3. BE AN ADVOCATE WITH THE PARENT.
Parents need to know that we are on the same side as them. We are truly a TEAM for their child. It is sometimes difficult to convey this message if/when our parents have been in IEPs that felt anything but supportive in the past and they come into the new IEP on the defensive. This is when we really need to reach out to them. I had so many nurses and doctors telling me how great the other hospital facility would be (and it was with more space and less noise) but they kept the pressure on to move my child even when I expressed my concern over and over. The doctor that brought her into the world ended up being my biggest support an ally. While everyone else pressured me to move her and let them put her on formula, he shared with me (as a grandparent) that my decision was really the best for her. He encouraged me and backed me up against the suggestions of the other hospital staff.
4. THEY ARE OUR KIDS TOO.
Every child on my caseload becomes my child too. I want the best for them. Therefore, I provide the services that I would want another service provider to provide if it truly was my child. We spent nearly 3 months in the NICU. During that time, my child became eligible for early intervention services and supports and financial assistance for all of her medical care. I knew these services were available due to my years of service in special education. Not once did the case manager inform us of services that she qualified for or to refer her for these services. In fact, I had to request the information and referrals to be sent to the appropriate services. We need to educate parents on what additional outside services are available or the process to determine eligibility for additional services.
5. ALWAYS EXPLAIN and GIVE EXAMPLES.
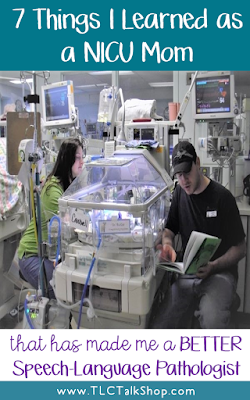 We are use to our jargon. Unfortunately, sometimes we are unable to avoid using jargon. When we have to use it, we need to give examples. For example, when we are discussing with a parent about the different types of stuttering or the techniques to modify stuttering or to shape fluency, we need to give examples. It doesn’t do any justice using other words to explain. If you can give an example or a visual it can help. As I sat there providing kangaroo care to my child (skin on skin contact), she had many desat episodes due to apnea. All I knew was that bells would ring and her little monitor would go crazy. Staff had to explain that desat and apneic episodes meant that she stopped breathing and how to read the monitor so that I would not jump every time it rang but when it was important to call out for assistance.
We are use to our jargon. Unfortunately, sometimes we are unable to avoid using jargon. When we have to use it, we need to give examples. For example, when we are discussing with a parent about the different types of stuttering or the techniques to modify stuttering or to shape fluency, we need to give examples. It doesn’t do any justice using other words to explain. If you can give an example or a visual it can help. As I sat there providing kangaroo care to my child (skin on skin contact), she had many desat episodes due to apnea. All I knew was that bells would ring and her little monitor would go crazy. Staff had to explain that desat and apneic episodes meant that she stopped breathing and how to read the monitor so that I would not jump every time it rang but when it was important to call out for assistance. 6. LISTEN and PROVIDE SUPPORT.
IEPs can be scary. Some parents have to go through a grieving process when their expectations for their child’s future may not be a reality or they are unsure if it can every be a reality. I spent 18 hours a day in that NICU holding my child, watching other parents come and go with their babies, and wondering when it would be our turn and what the future may be for her. Why did other parents get to take their babies home after a day, a week, or a month and I had to sit there day after day? What would her future look like? Would she have academic concerns? Would she always have a heart murmur or any heart problems? I was fortunate enough that the NICU nurses were spectacular. They listened to my fears. They cried with me and they gave me encouragement. We need to do this with our parent’s fears too. We need to listen, be empathetic, and provide support.
7. ENCOURAGE PARENTS to BRING THEIR SUPPORT SYSTEM to IEPS.
Yes, that includes advocates if parents feel that they need that level of support. Grandparents, siblings, advocates, prior service providers, etc.. anyone that makes the parent feel supported during the process. By encouraging and accepting others into the meeting, we are letting the parent know that we really do consider them a part of the IEP TEAM and that we do have their child’s best interests at heart. For my little one to come home she had to be able to take so many meals by bottle within a certain time period. When the hospital staff sent someone to discuss the matter with me and help me to help her with this task, they sent an Occupational Therapist. I appreciate my fellow service providers; however, being a Speech-Language Pathologist I was most comfortable with and made a special request for another Speech-Language Pathologist.. They could have very easily rolled their eyes, gave me a million reasons why the OT was just as capable, and gave me a difficult time about my request. They didn’t. They were supportive so it made me feel empowered and part of my child’s team.
What life experiences do you feel has made you a better SLP? What lessons did you learn? I would love for you to share your experiences that helped you grow into the therapist that you are today in the comments below. We all grow as a discipline when we actively reach out to educate ourselves and share with others.
Want more great tips, tricks, and ideas for successful speech therapy? Subscribe to our , or visit us on Instagram, Pinterest, or Facebook.
Want more great tips, tricks, and ideas for successful speech therapy? Subscribe to our , or visit us on Instagram, Pinterest, or Facebook.





